The first step in haemodialysis is a relatively simple surgery to create access to your blood vessels.
This usually only needs to be done once, as the access stays in place for your treatments, and is usually done a few weeks before your first dialysis session. Access is created in one of three ways: by a fistula, whereby a direct connection is made between an artery and a vein, creating a strong vessel to withstand the regular insertion and removal of needles; by a graft, whereby a similar connection is made indirectly via a plastic tube; by a Y-shaped catheter, where a plastic tube is inserted directly into a larger vein. If you have a fistula or graft, at the start of each HD treatment, two needles are placed into the vascular access, one allowing blood to flow into the dialysis machine, and one allowing it to flow back into your body from the machine.
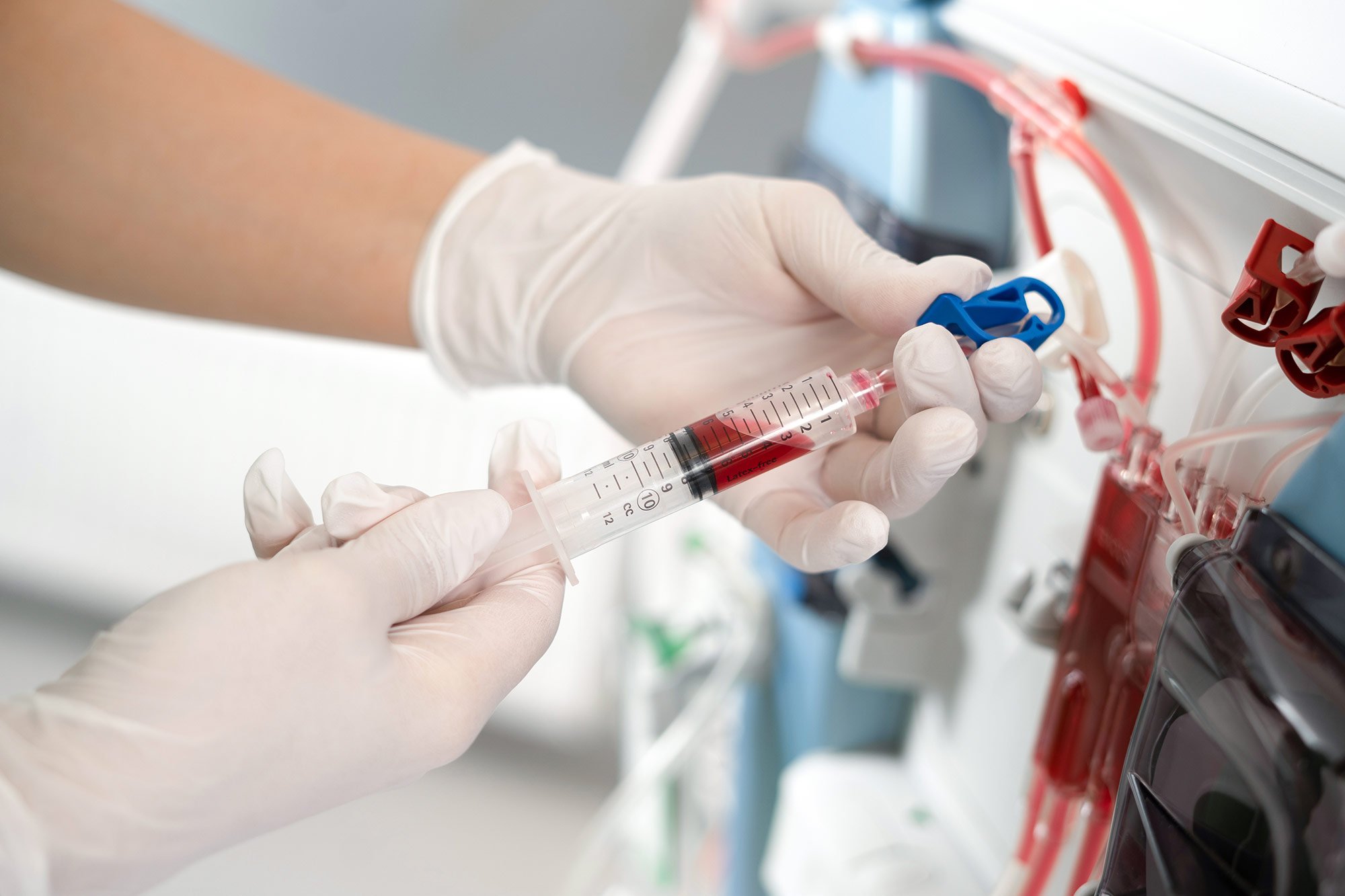
Sterile plastic tubes (bloodlines) carry your blood into the dialysis machine. The key part of this machine is the dialyser, a series of thin semipermeable membranes which acts as a barrier between your blood and the dialysis fluid. These membranes allow substances to move out of and into your blood and in this way waste products and excess water are removed from your body and medication may also be given. The dialysis circuit carries blood at 200-300 ml/min, flow at >350ml/min. A complete dialysis session usually takes 4-5 hours and is repeated at least 3 times every week.

You are encouraged to relax during the dialysis treatment, by reading, sleeping, working, watching television etc. Nurses will keep a very close eye on you throughout your dialysis and ensure that the machine is working correctly.
Dialysis should not be painful, but it is common to feel tired afterwards, a side-effect which can be alleviated by adjusting your diet and taking regular exercise. You may feel sick, dizzy or have muscle cramps during dialysis, and are always encouraged to seek help from our medical teams.
Home haemodialysis
In some countries, Diaverum offers haemodialysis that you can do at home. We will provide you with a special dialysis machine that treats your domestic water so it is suitable for dialysis, and all the supplies you need will be delivered to your home once or twice a month. You will be taught how to use the machine in a series of sessions at the clinic, usually over 8-12 weeks. You are also welcome to bring a helper to these sessions who can then support you at home.
During training, you will learn to:
- prepare equipment and supplies
- place the needles in the vascular access (fistula or graft)
- administer medication
- monitor the machine
- check your blood pressure and pulse
- keep treatment records
- clean the equipment and room where you do your dialysis
- order supplies
Home haemodialysis can make your life more flexible, as you can set your own schedule to fit with other activities, such as going to work or caring for a family member. You may also choose to do dialysis more often than if you had to go to the clinic, which may mean:
- you feel better and have better blood pressure control
- you have less restriction on diet and fluids
- you save time travelling to and from the clinic - they will usually review you there once a month
- you will need a space where the machine can be set up
- you will need space to store all the supplies you need for your treatments
Self-care or shared-care haemodialysis
As well as haemodialysis in the clinic or at home, we also support patients who want a middle-ground between these two options.
In self-care or shared-care haemodialysis, you can learn to do some of your dialysis treatment at the clinic. You will agree a training plan with our staff, and then gradually learn different skills. It is up to you to decide how much of the process you feel comfortable to learn, and the approach will be regularly reviewed with you.
Tasks you can learn to do during training for self- or shared-care dialysis include:
- preparing equipment and supplies
- placing the needles in the vascular access
- administering medication
- monitoring the dialysis machine
- checking blood pressure and pulse
- keeping treatment records
- more control over your treatment and greater independence
- increased understanding of and improved management of CKD
- greater flexibility of dialysis schedules and time-saving